Why families hesitate, why timing matters, and how to act before crisis forces the decision
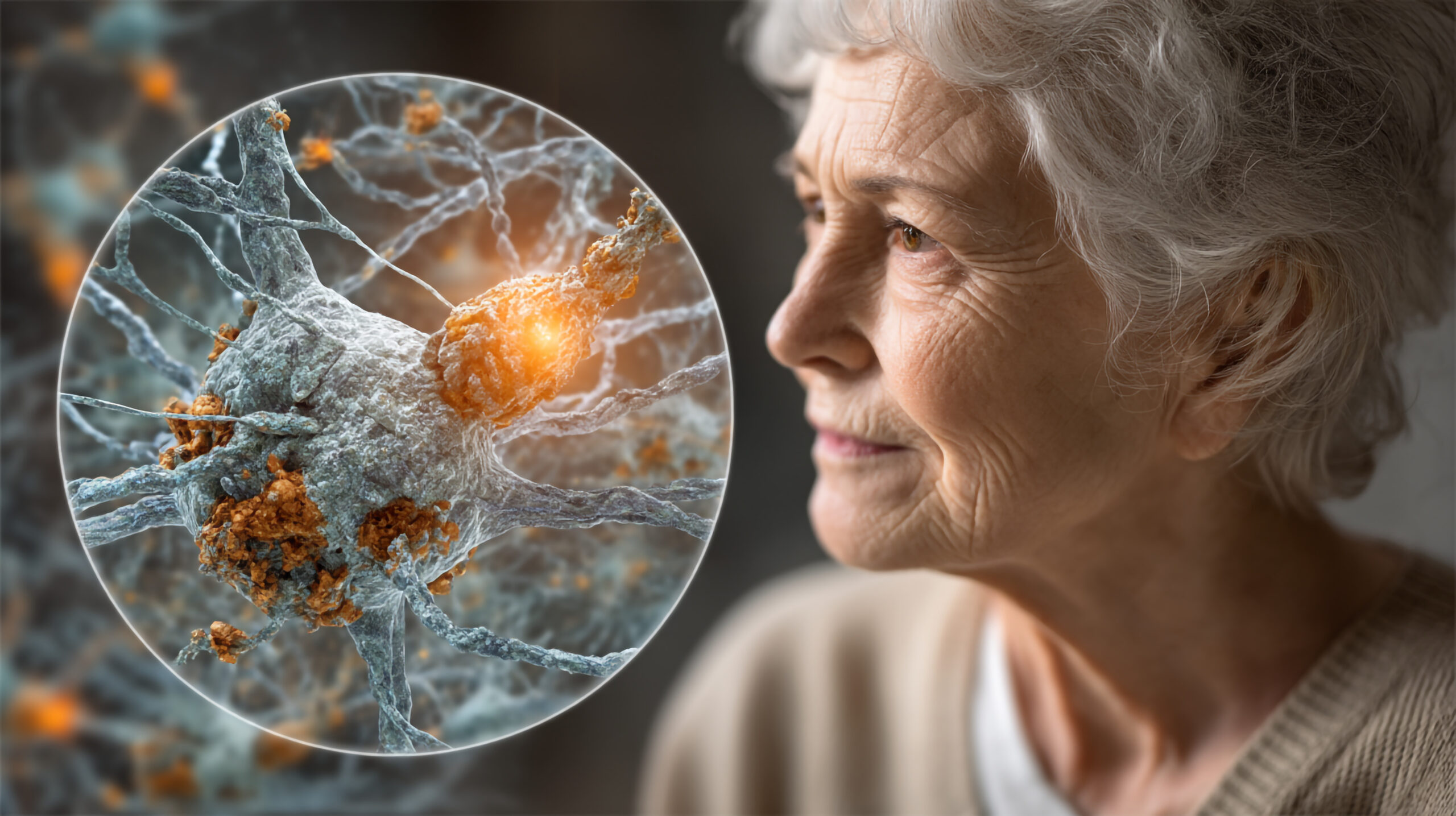
Memory problems rarely begin in obvious ways. For most families, the earliest changes are subtle and easy to dismiss. They tend to appear as small disruptions in daily life rather than clear or dramatic memory loss.
From a clinical perspective, this early phase is often the most challenging, not because the changes are severe, but because they are ambiguous. Families are left asking quiet questions: Is this normal aging? Stress? Depression? Or something more concerning? There is rarely a single moment when uncertainty turns into clarity.
Early cognitive changes are often the first indication that a family may eventually need to think about safety, supervision, and long-term support. Recognizing these changes early allows time for understanding and planning, before decisions are driven by urgency or crisis.
What Families First Notice and Why It’s So Easy to Look Away
A loved one may begin repeating stories, mismanaging bills, missing appointments, or relying increasingly on notes and reminders. Conversations may feel harder to follow. Judgment may seem subtly less reliable. Some families notice changes in mood or personality, irritability, withdrawal, or a loss of initiative that feels unfamiliar.
Because these changes unfold gradually, families often attribute them to normal aging, stress, grief, or distraction. Everyone forgets things. Life is busy. Waiting feels reasonable.
This tendency to minimize early memory changes is rarely neglect. More often, it reflects emotional self-protection. Acknowledging cognitive change raises uncomfortable questions about independence, safety, and the future. For many families, uncertainty feels more tolerable than clarity. There is also a common fear that seeking evaluation will immediately force decisions they are not ready to make.
Yet clinically, waiting often makes things harder.
The Cost of Unexamined Change
When memory or thinking changes go unexamined, potentially treatable contributors may be missed. Medication side effects, sleep disorders, depression, metabolic abnormalities, and other medical conditions can all affect cognition. Without careful evaluation, these factors may quietly worsen or be misattributed solely to aging.
Over time, safety risks tend to increase gradually rather than suddenly. Errors involving medications, finances, nutrition, or daily activities often appear long before a major event occurs. Families frequently recognize the pattern only in retrospect.
Many people seek help after a fall, a financial mistake, or a sudden behavioral change forces action. At that point, decisions often feel rushed, emotional, and overwhelming. What feels like a sudden decline is usually the culmination of changes that have been unfolding quietly for months or years.
Evaluation Is About Understanding, Not Conclusions
Seeking a cognitive evaluation is not about rushing to a diagnosis or assuming the worst. It is about understanding what is happening.
An evaluation is appropriate when changes persist, interfere with daily responsibilities, or are observed by more than one person. Changes in judgment, behavior, or mood should prompt attention even when memory loss itself seems mild.
A careful assessment can help distinguish normal aging from medical causes or neurocognitive illness. It allows potentially reversible factors to be identified and treated. Just as importantly, it establishes a baseline for better assessing future symptoms and the efficacy of current and future interventions.
Independence, Safety, and Timing
Families sometimes feel that seeking evaluation may lead to loss of independence for the individual. In reality, earlier understanding often helps preserve independence longer. It allows families to plan gradually and adapt supports thoughtfully, rather than having to pull resources together in the midst of a crisis.